Author: Claire Tian
Editor: Rebecca Ting
Revised: Dina Abbas, Helia Mansouri Dana
Overview
The SARS-CoV-2 coronavirus is a newly emerged viral strain that has been responsible for the notorious pandemic, causing the disease referred to as COVID-19 (Wang, Zhao, Gao, et al., 2020). COVID-19 and the associated hassles it entails such as physical distancing is further exacerbated and appears to perpetuate seemingly endlessly due to the ease of transmissibility of the virus (Harrison, Lin, & Wang, 2020).

The origin of this pandemic began in December 2019, when several patients were reportedly afflicted with severely heightened symptoms resembling that of the common cold (Harrison, Lin, & Wang, 2020). The SARS-CoV-2 virus instantly became pervasive following multiple occurrences of direct human-to-human contact (Harrison, Lin, & Wang, 2020).
Treatment options such as drug therapeutics are currently being developed, though vaccinations are currently the best mode of action in ensuring public health and safety (Wang, Zhao, Gao, et al., 2020).
Find more information about the COVID-19 status around the world on the COVID-19 Dashboard
What causes COVID-19?
On a biochemical level, the SARS-CoV-2 virus possesses more or less the same receptors as those of the SARS-CoV, which allows them to attach to multiple host cells, such as in pigs, dogs, rabbits, cats, and the rhesus monkeys (Hu, Guo, Zhou, et al., 2021), thereby facilitating the viral infection process. This transmission is further aided in humans upon their interactions with already infected animals (Bakhiet & Taurin, 2021).
SARS-CoV-2 appears to be widespread throughout the world, particularly due to its easy nature of transmission from human to human; specifically, through minute air droplets (Wang, Zhao, Gao, et al., 2020). In simple words, upon sneezing into the open air, where droplets travel rapidly, followed by individuals within the vicinity inhaling it into their bodies (Wang, Zhao, Gao, et al., 2020).

The bacteria and virus in droplets also reside on many surfaces for extended periods of time, which can then infect humans upon direct contact via their hands and touching their face; this action causes the virus to enter the sinuses and the respiratory tracts through the throat (Wang, Zhao, Gao, et al., 2020).
Due to the easy nature of transmission of the SARS-CoV-2 virus, there is no doubt that COVID-19 spreads very quickly among populations, especially among regions where there are more individuals concentrated in one area (Harrison, Lin, & Wang, 2020).
Symptoms
- Fever
- Persistent coughing (dry cough)
- Pain or tightening sensation or discomfort in the chest
- Ongoing difficulty with breathing
- Pneumonia
- Headaches, dizziness, nausea, impaired consciousness
- General fatigue
- Loss of sense of smell and taste
(Böger, Fachi, Vilhena, et al., 2021; Wang, Li, Yan, et al., 2020)
Risk Factors
- Smoking
- Obesity and/diabetes association )
- Living in heavily air polluted environments
- Age (with seniors being at the highest risk of infection and mortality )
- Underlying or preexisting chronic lung diseases/heart complications
(A. B. Engin, E. Engin, & A. Engin, 2020)
How is COVID-19 Diagnosed?
A diagnosis of SARS-CoV-2 infection is typically determined through oropharyngeal (centre throat) swab test as well as obtaining a sample of the patient’s blood, urine, or anal (Peng, Liu, Xu, et al., 2020). These bodily fluid samples are then tested for the presence of the SARS-CoV-2 virus (Peng, Liu, Xu, et al., 2020).
The SARS-CoV-2 virus predominantly affects the entirety of the respiratory tract, including both upper and lower; therefore, some of the quickest and convenient methods of detecting potential COVID-19 usually involve nasopharyngeal and anterior nasal swabs (upper respiratory tract testing) (Lai & Lam, 2020).
Testing of the upper respiratory tract can be performed for detection of the early stages of COVID-19, while testing of the lower respiratory tract is suitable for patients who are suspected to be infected with COVID-19 but have tested negative with the samples collected from the upper respiratory tract (Lai & Lam, 2020).
To a lesser extent, blood samples (the plasma portion) may occasionally be used to detect SARS-CoV-2 infection in patients who are entering the critical stage of the disease; however, these have limited efficacy in clinical diagnosis (Lai & Lam, 2020).
Prevention & Vaccination
The best form of intervention is to become fully vaccinated against the virus; this means acquiring two doses of the Pfizer BioNTech, Moderna, or other approved vaccines, as noted by the CDC (Pilishvili et al., 2021; Tenforde et al., 2021).
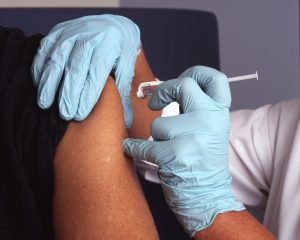
In addition, physical distancing measures, as well as wearing a mask that covers the nose and mouth (ie. preventing entry of potential viruses and contaminants into the respiratory tract) and sanitizing/washing the hands is essential in further prevention of contracting the virus (Alvi, Sivasankaran, & Singh, 2020).
Treatment
Currently, there are many management and treatment strategies in development or undergoing active clinical trial testing (Toor, Saleh, Nair, et al., 2020). One example would be adoptive T-cell therapy, which aims to recover immunity and helps prevent future viral infections (Toor, Saleh, Nair, et al., 2020).
There are also antiviral molecules that work to inhibit the SARS-CoV-2 virus from entering the host cell, thereby preventing infection entirely, to begin with (Oroojalian, Haghbin, Baradaran, et al., 2020). These molecules work by interfering with the chemical interaction between the spike protein and its receptors on the host cell (Oroojalian, Haghbin, Baradaran, et al., 2020).
Furthermore, antiviral drugs are in the ongoing stages of development, such as protease inhibitors, oseltamivir, and hydroxychloroquine (Oroojalian, Haghbin, Baradaran, et al., 2020). Vaccines such as AstraZeneca, Pfizer, and Moderna, among many others, are also undergoing clinical trial testings with their efficacies being monitored in the general population (Oroojalian, Haghbin, Baradaran, et al., 2020).
For patients who are already infected with the SARS-CoV-2 virus, hospital beds and ventilators are common and crucial non-pharmacological methods of preserving adequate breathing (life) and at the very least, supposedly prevent further respiratory complications (Alvi, Sivasankaran, & Singh, 2020).
References
Alvi, M., Sivasankaran, S., & Singh, M. (2020). Pharmacological and non-pharmacological efforts at prevention, mitigation, and treatment for COVID-19. Journal of Drug Targeting, 28(7-8), 742-754. https://doi.org/10.1080/1061186X.2020.1793990
Bakhiet, M., & Taurin, S. (2021). SARS-CoV-2: Targeted managements and vaccine development. Cytokine & Growth Factor Reviews, 58, 16-29. https://linkinghub.elsevier.com/retrieve/pii/S1359610120302276
Boger, B., Fachi, M., Vilhena, R., Cobre, A., Tonin, F., & Pontarolo, R. (2021). Systematic review with meta-analysis of the accuracy of diagnostic tests for COVID-19. American Journal of Infection Control, 49(1), 21-29. https://linkinghub.elsevier.com/retrieve/pii/S0196655320306933
Engin, A.B., Engin, E.D., & Engin, A. (2020). Two important controversial risk factors in SARS-CoV-2 infection: Obesity and smoking. Environmental Toxicology and Pharmacology, 78, 1-7. https://linkinghub.elsevier.com/retrieve/pii/S1382668920300879
Harrison, A., Lin, T., & Wang, P. (2020). Mechanisms of SARS-CoV-2 Transmission and Pathogenesis. Trends in Immunology, 41(12), 1100-1115. https://doi.org/10.1016/j.it.2020.10.004
Hu, B., Guo, H., Zhou, P., & Shi, Z. (2021). Characteristics of SARS-CoV-2 and COVID-19. Nature Reviews. Microbiology, 19(3), 141-154. https://doi.org/10.1038/s41579-020-00459-7
Lai, C., Lam, W. (2021). Laboratory testing for the diagnosis of COVID-19. Biochemical and Biophysical Research Communications, 538, 226-230. https://doi.org/10.1002/jmv.25936
Oroojalian, F., Haghbin, A., Baradaran, B., Hemmat, N., Shahbazi, M., Baghi, H., Mokhtarzadeh, A., & Hamblin, M. (2020). Novel insights into the treatment of SARS-CoV-2 infection: An overview of current clinical trials. International Journal of Biological Macromolecules, 165, 18-43. https://doi.org/10.1016/j.ijbiomac.2020.09.204
Peng, L., Liu, J., Xu, W., Luo, Q., & Chen, D., Lei, Z., Huang, Z., Li, X., Deng, K., Lin, B., & Gao, Z. (2020). SARS-CoV-2 can be detected in urine, blood, anal swabs, and oropharyngeal swabs specimens. Journal of Medical Virology, 92(9), 1676-1680. https://doi.org/10.1002/jmv.25936
Pilishvili, T. (2021). Interim Estimates of Vaccine Effectiveness of Pfizer-BioNTech and Moderna COVID-19 Vaccines Among Health Care Personnel—33 U.S. Sites, January–March 2021. MMWR. Morbidity and Mortality Weekly Report, 70. https://doi.org/10.15585/mmwr.mm7020e2
Tenforde, M. W. (2021). Effectiveness of Pfizer-BioNTech and Moderna Vaccines Against COVID-19 Among Hospitalized Adults Aged ≥65 Years—United States, January–March 2021. MMWR. Morbidity and Mortality Weekly Report, 70. https://doi.org/10.15585/mmwr.mm7018e1
Toor, S., Saleh, R., Sasidharan, V., Taha, R., & Elkord, E. (2021). T-cell responses and therapies against SARS-CoV-2 infection. Immunology, 162(1), 30-43. https://doi.org/10.1111/imm.13262
Wang, H., Li, X., Yan, Z., Sun, X., Han, J., & Zhang, B. (2020). Potential neurological symptoms of COVID-19. Therapeutic Advances in Neurological Disorders, 13, 1-2. http://journals.sagepub.com/doi/10.1177/1756286420917830
Wang, M., Zhao, R., Gao, L., Gao, X., Wang, D., & Cao, J. (2020). SARS-CoV-2: Structure, Biology, and Structure-Based Therapeutics Development. Frontiers in Cellular and Infection Microbiology, 10, 1-17. https://doi.org/10.3389/fcimb.2020.587269
